Diabetic Eye Disease: What You Need to Know
April 9, 2020
What Is Diabetic Eye Disease?
Diabetes, a metabolic disorder where the body has elevated blood sugar levels for prolonged periods of time, can have a dramatic effect on your health. This includes the health and function of your eyes, as diabetes and eyesight are interconnected. Diabetes is one of the leading causes of irreversible blindness worldwide, and in fact, it is the most common cause of blindness in people younger than 65 in the United States.
“Diabetic eye disease” is a group of eye problems brought on or worsened by diabetes that can have a significant, negative impact on your eyes over time. These problems can include:

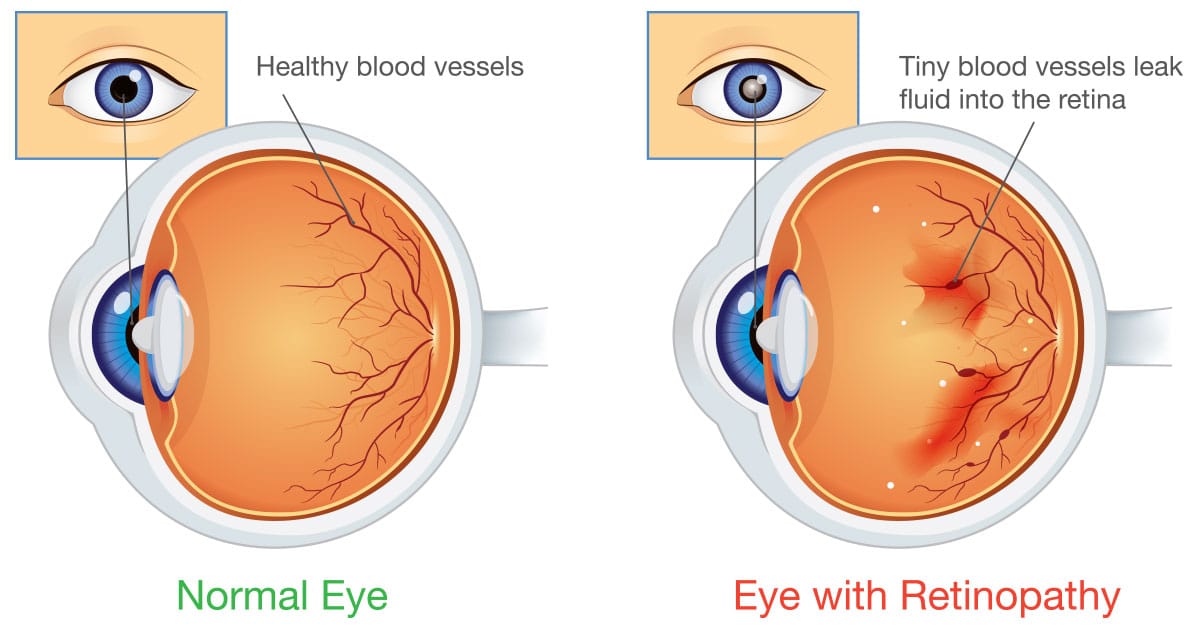
Diabetic Retinopathy
What Is Diabetic Retinopathy?
This is a condition that causes eye problems for people with diabetes, all centered around damage being caused to the blood vessels of the light-sensitive tissue of the retina. This is the core issue with blurry vision from diabetes and diabetes blindness.
What Is the First Sign of Diabetic Retinopathy?
Symptoms are often not present in the early stages of retinopathy. Once a person with diabetic retinopathy begins to experience changes in vision, they are likely already in advanced stages of retinopathy and the chances of having irreparable damage to vision are high. This underscores the importance of undergoing eye examinations regularly if you are diabetic. First noticeable symptoms may include spots or dark floaters, blurred vision, fluctuating vision, impaired color vision, or dark or empty areas in your vision.
What Are the Four Stages of Diabetic Retinopathy?
The four stages of diabetic retinopathy are classified as mild, moderate, severe nonproliferative, and proliferative.
- Mild Nonproliferative Diabetic Retinopathy — In this initial stage, microaneurysms in the form balloon-like swelling in small areas of the retina’s blood vessels occur.
- Moderate Nonproliferative Diabetic Retinopathy — Blood vessels that nourish the retina become blocked.
- Severe Nonproliferative Diabetic Retinopathy (NPDR) — The retina is no longer receiving adequate blood flow, as more blood vessels become blocked.
In these early stages of diabetic eye disease, damaged blood vessels can weaken, bulge, and leak fluids (including small amounts of blood) into the retina. This can cause the retina and macula to swell and cause vision loss.
When affected by diabetic retinopathy you can develop macular ischemia, a condition where the blood vessels in the retina can close off and prevent blood flow to the macula. As the macula is not receiving enough blood and oxygen to work properly, macular ischemia can cause damage within the retina and contribute to blurred vision.
- Proliferative Diabetic Retinopathy (PDR) — In more advanced stages of diabetic eye disease the retina starts growing new blood vessels. These vessels may cause bleeding behind the eye into the vitreous cavity of the eye at varying degrees, causing adverse vision effects from dark floaters to full loss of vision.
The new blood vessels generated from PDR can create scar tissue as well, leading to additional problems with the macula or a detached retina (which typically causes blindness and can only be treated with surgery).
Diabetic Macular Edema
Diabetic maculopathy (damage to the macula) can be a result of retinopathy. This commonly manifests as a diabetic macular edema (DME), caused by fluid build-up in the macula.
- Diabetic macular edema (DME) represents the specific condition of fluid accumulating in the macula, causing swelling. Since the macula is filled with cells that are responsible for sharp, straight-ahead vision, the swelling brought on by DME can impair the ability of those cells and cause blurred vision and washed-out colors.
Cataracts
- A cataract is a clouding of the natural lens of the eye, often obstructing light from entering the eye and commonly results in blurred vision and/or glare. Cataracts are a natural part of the aging process but can be expedited by uncontrolled diabetes.
Glaucoma
- Glaucoma is a condition linked to a buildup of high intraocular pressure (or fluid pressure inside the eye). As pressure increases over time, damage can be caused to your eye’s optic nerve and can cause vision loss or blindness. While eye drops may be prescribed to lessen fluid production and increase the outflow of fluid from the eye, surgery can be necessary to halt the progression of the disease. Glaucoma is known as “the silent thief of sight” because there are often no symptoms until the condition is so advanced that vision loss has already occurred.
The Path to Clearer Vision Starts Here
What Is a Diabetic Eye Exam?
The only way to truly diagnose diabetic retinopathy is to have a dilated eye exam. An ophthalmologist will put drops in your eye to dilate your pupils. This dilation, along with a special magnifying lens, allows the doctor to examine a larger area at the back of each eye and inspect for damage caused by retinopathy.
While your eyes are dilated, the ophthalmologist might (but not always) opt to do further testing to gain more information.
- Optical coherence tomography (OCT) provides a high-resolution image of the layers of the retina, similar to an ultrasound. This allows the doctor to assess the health of the retina. Among other things, it will show leaking blood vessels, hemorrhages, or areas where the retina has been damaged by ischemia.
- Fluorescein angiography allows your doctor to identify which blood vessels have blockages and which vessels leak blood. This is achieved by injecting a special dye into your arm while your eyes are dilated.
In addition to these tests, your ophthalmologist will also check your unassisted vision as well as your eye pressure to help get a more comprehensive analysis of your eye health and assess any areas of concern.
How Can You Tell If Diabetes Is Affecting Your Eyes?
Diabetes often has a progressive effect on your eyes and vision. This means that during early stages you may not have any symptoms or they may be mild or barely noticeable. Unfortunately, eye disease with diabetes can worsen over time and lead to severe vision loss if left untreated. This is why it is important for you to have an eye exam every year, especially if you are experiencing diabetic eye problems.
Common diabetic eye symptoms may include:
- Floaters, or dots and dark strings, in your field of vision
- Dark or empty areas in your field of vision
- Blurry vision
- Difficulty focusing
- Vision changes that seem to fluctuate
- Poor night vision
- Noticing that colors appear faded or washed out
- Partial or total vision loss
Is Diabetic Eye Disease Reversible?
It is possible for early stages of diabetic retinopathy to be treated and reversed. Once a person reaches the later stages, they are at risk of permanent vision changes, loss, or scarring due to lack of blood flow and oxygenation.
The primary treatment for reversing diabetic eye disease is controlling your blood sugar levels, reducing high blood pressure, and generally managing your diabetes. Maintaining a healthy weight and eating a well-balanced diet can help improve your insulin sensitivity and lower your blood sugar levels. Consistent dilated eye exams will help you stay informed of your eye health and even catch problems before symptoms begin. Addressing health issues early is the key to avoiding irreversible damage to vision.
Conclusion
If you have diabetes, you are at risk for vision problems. Managing your overall health and controlling your diabetes is vital to retaining healthy vision. If you know you have diabetes and blurred vision is occurring, or if you are experiencing other symptoms related to diabetic eye disease, please contact us. The experienced, Board Certified Ophthalmologists at Heart of Texas Eye Institute are here to help you with the exams you need and help put together a treatment plan.