Three Types of Cataracts and Their Treatments
October 31, 2020
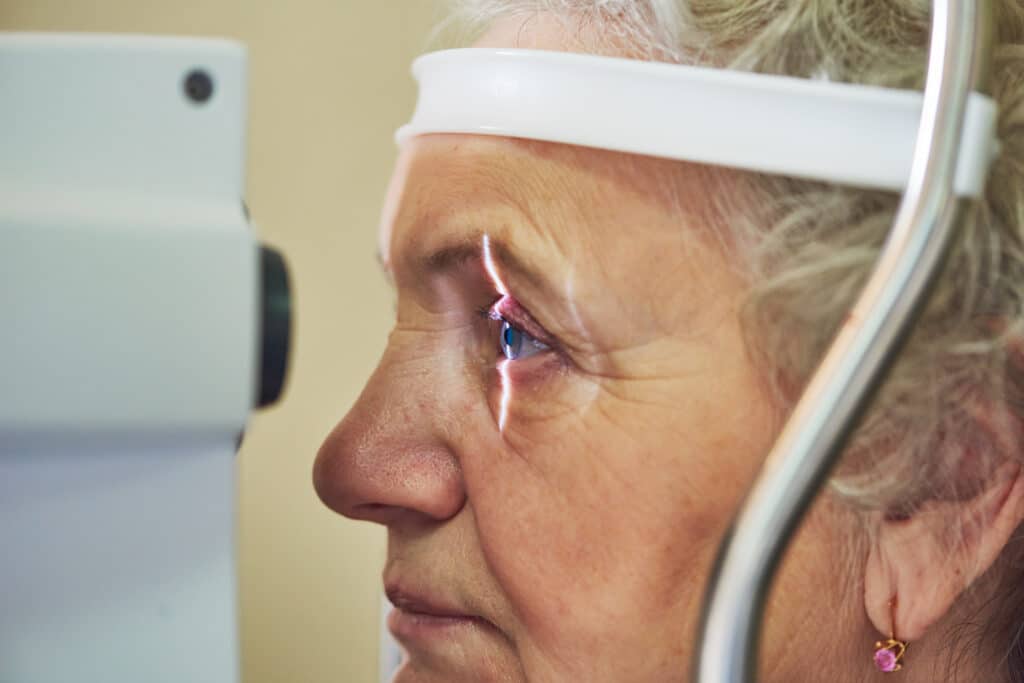
What Is a Cataract?
A cataract is the buildup of proteins in the lens within the eye. This protein buildup creates cloudiness and opacity within the lens. In turn, the vision becomes blurred, hazy, faded or generally worsened. Cataracts are a highly common condition that can occur naturally, typical as we get older. In America, more than 24.4 million people over age 40 are affected by cataracts, and half of those who are 75 or older either have had cataracts or had them surgically removed.
Cataracts are not always caused by age, however. They can be brought on by injuries to the eye, medical conditions such as diabetes, eye surgeries or other eye conditions. The use of steroids may hasten the progression of cataracts. Though relatively uncommon, children are sometimes born with congenital cataracts or develop them during childhood. Thankfully, regardless of their cause, cataracts can be treated surgically with a high degree of success.
Interestingly enough, not all cataracts are the same. Each type of cataract forms in a specific portion of the lens with varying physical effects and progression patterns.
What Are the Three Main Types of Cataracts?
Posterior Subcapsular Cataracts (Back of Lens)
Posterior Subcapsular Cataracts (PSC) form in the back of the lens, aside the capsule which holds the lens in place. As the cataract develops, it will increasingly obstruct the path of light and cause glare. This type of cataract is commonly found in patients who have had eye trauma or surgery, who have had elevated blood sugar levels, or who have been treated with steroids. However, a PSC cataract can form in perfectly normal eyes who do not meet any of these criteria. Occasionally, PSC cataracts will be present in children and even infants.
The progression of a PSC cataract is typically more rapid than other forms of cataract. It may become visually significant over the course of months or years, but can happen as quickly as weeks and even days.
PSC cataracts can compromise one’s reading vision, cause glare or halos around lights during the night, and may result in worsened vision in bright-light settings. If left untreated, posterior subcapsular cataracts may result in significant impairment of vision and can progress to the point of blindness.
The Path to Clearer Vision Starts Here
Nuclear Sclerosis Cataracts (Center of Lens)
The nuclear sclerotic cataract (also known as a “nuclear cataract”) is the most common type of cataract and it generally is brought on as a result of advancing age. Nuclear cataracts affect the center of the lens, also known as the nucleus. With this type of cataract, the lens gradually hardens and turns densely yellow or brown over time. This hardening of the lens is referred to as “sclerosis.” An oddity with this condition is that in the early stages some patients report sudden vision improvements, including improvements in nearsightedness or reading vision. However, this effect (commonly referred to as “second sight”) is only temporary. In general, nuclear cataracts cause more significant impairment on distance vision than near vision.
As a nuclear cataract reaches advanced stages, it can make it difficult for the patient to distinguish between different shades of color. Thankfully, the nuclear sclerotic cataract grows slowly and may take several years until it begins to impact one’s vision in a dramatic way. Many patients are able to delay cataract surgery with effective reading glasses and eyeglasses, wearing anti-glare sunglasses, and taking precautions such as avoiding night driving.
Cortical Cataracts (Outer Layer of Lens)
A cortical cataract affects the outer layer of the lens. This type of cataract occurs when opacities are formed in the lens cortex. The cortical cataract is noticeable in early stages when small clouded areas or white streaks begin to form within the lens cortex. These white streaks, (also known as “cortical spokes”) can grow to extend to the center of the lens as the cortical cataracts worsen. When this occurs, the streaks may block light from naturally passing through the lens which can cause glares, light sensitivity, blurred vision, and problems with depth perception. Prescription eyeglasses may help make up for some vision loss in the short term, but cataract surgery will eventually be needed to correct this condition.
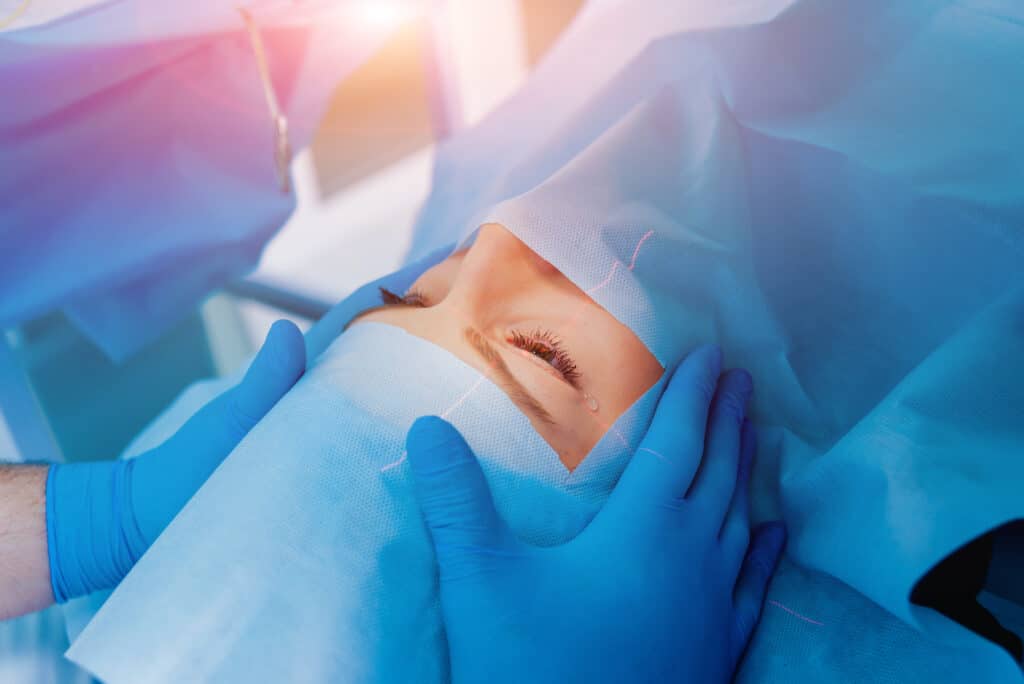
How Are Cataracts Treated?
Getting treatment is essential when you begin to notice changes in your vision, symptoms related to cataracts, or visual signs of cataracts. If left untreated, cataract surgery may become more challenging in the advanced stages of cataract formation, This may limit a patient’s surgical options or necessitate multiple surgeries. If left untreated, cataracts will progress to the point where they lead to blindness over time, Cataracts remain one of the leading causes of blindness. However, proper treatment can fully remove cataracts, improve the vision, and potentially clear away the need for glasses at the same time.
Depending on the lens options that are chosen for the surgery, glasses may or may not be necessary following surgery.
With each of the different types of cataracts, cataract surgery is necessary to treat the condition and restore vision for a patient. Fortunately, surgery to correct cataracts is very common, safe, and effective. It is typically an outpatient surgery that is completed in 30 minutes or less (per eye) and generally only requires numbing drops and minimal sedation. The surgery involves the removal of the natural lens affected by a cataract, followed by the placement of an artificial lens. The vision should begin improving within a matter of days as the eye heals and adjusts to its new lens. While complete healing may take several weeks, everyday activities should be able to be resumed within a few days of the procedure with very little restriction.
Conclusion
While these different types of cataracts can affect vision in slightly different manners, all of them can lead to significant loss of vision (even blindness) over time. Regardless of the variation, cataracts can easily be removed and prevented from recurring through surgery. If you are experiencing issues or abnormalities with your vision it is important to schedule an appointment with your eye doctor to provide further guidance. If you do have cataracts, your options for cataract surgery should be discussed. Before deciding anything, read our blog to know see what should be considered before getting cataract surgery and be sure to look into the do’s and do nots of post cataract surgery.
At Heart of Texas Eye Institute, we are committed to delivering the best outcomes possible for our patients. Both of our board-certified ophthalmologists have combined experience of over 100,000 procedures and are industry leaders in cataract and refractive surgery. This means that regardless of the type of cataract a patient is experiencing, we are able to address the condition and provide highly informed recommendations for each unique situation. If cataracts have begun to form or if you are experiencing issues with your vision, please reach out to us for a cataract consultation.